Previous Article
Understanding Chronic Pain and Treatments
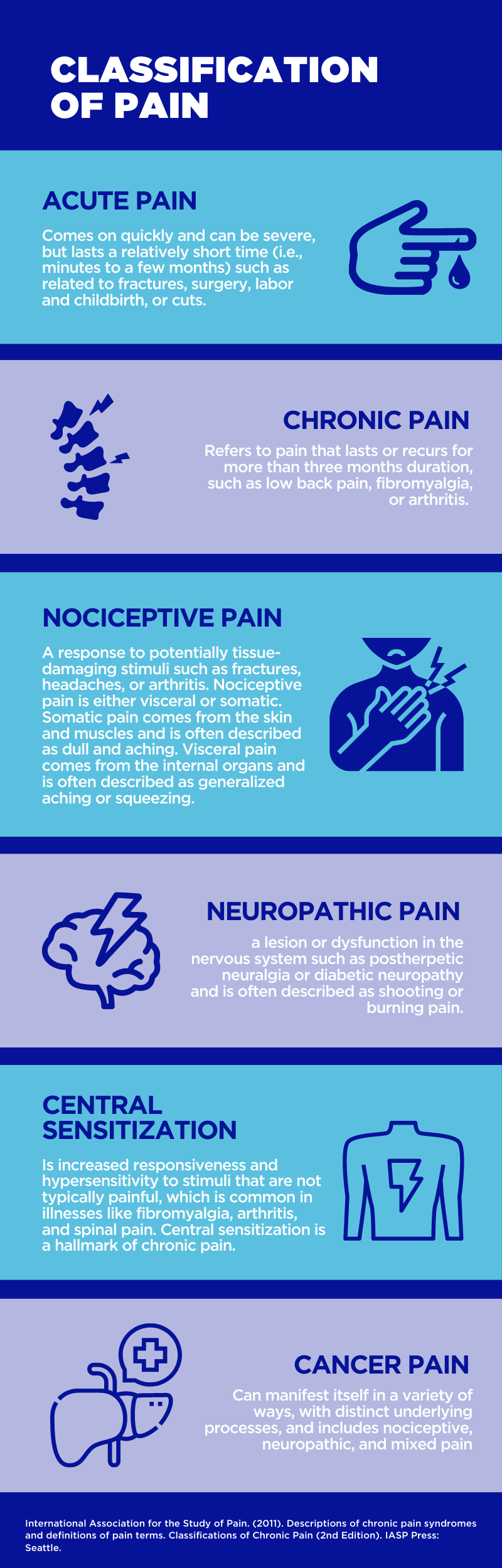
Pain is critical in the survival of all animals including humans – it alerts us to potential tissue damage that leads to a wide range of actions to prevent or limit further damage.
Pain Physiology
Pain develops when sensory nerve endings termed nociceptors (i.e., pain receptors) meet a painful stimulus. The nerve impulse travels from the nociceptors to the spinal cord, where it is quickly diverted to the brain. The brain processes the pain sensation and quickly initiates a motor reaction to try to stop the action that is causing the pain1.
Pain that is persistent and recurring might become a concern and progress into chronic pain. We have learned that pain is a complicated interaction between various bodily functions that can fundamentally alter our nervous system. Most importantly, pain is influenced by biological, psychological, and social factors, leading the International Association for the Study of Pain (IASP) to define pain as “an unpleasant sensory and emotional experience associated with, or resembling that associate with, actual or potential tissues damage2.”
The Pain Triad
Chronic pain is rarely isolated; it is frequently linked with sleep disturbances and emotional distress, forming the well-known “Pain Triad”. These three interconnected ailments can affect a person's quality of life. For example, a high level of pain can lower your mood and reduce your quality of sleep.
The Analgesic Potential of Cannabinoids
Did you know that, like opioid receptors, we have 'cannabis receptors' in our brains? In fact, we produce substances like those found in cannabis in our bodies, which are known as 'endocannabinoids,' much as we produce opioids, which are known as 'endorphins.'
The endocannabinoid system interacts with opioid, serotonin, and NMDA receptors, which are all important pain pathways in our body.
CB1 and CB2 receptors are the two primary endocannabinoid receptors. CB1 receptors are found mostly in the peripheral and central nervous systems, and they have a direct overlap with opioid receptors. CB2 receptors regulate the release of cytokines, chemokines, neutrophils, and macrophages and are predominantly present in peripheral and immune cells, suggesting that these receptors have a key role in chronic inflammatory pain.3
References:
[1] International Association for the Study of Pain. (2011). Descriptions of chronic pain syndromes and definitions of pain terms. Classifications of Chronic Pain (2nd Edition). IASP Press: Seattle.
[2] IASP Definition of Pain Task Force. (2019). IASP’s proposed new definition of pain released for comment. Washington, D. C.: IASP. Retrieved from https://www.iasp-pain.org/PublicationsNews/NewsDetail.aspx?ItemNumber=9218|
[3] Cooper, Z.D., Bedi, G., Ramesh, D., Balter, R., Comer, S.D., & Haney, M. (2018). Impact of co-administration of oxycodone and smoked cannabis on analgesia and abuse liability. Neuropsychopharmacology, 43(10), 2046-2055.
Next Article
A Brief Overview on Canada’s Opioid Overdose Crisis
In Canada, the ongoing public health crisis of opioid overdose and deaths is worsening. Between January 2016 and June 2021, 24,626 persons died in Canada because of opioid overdoses, with latest figures indicating a frightening increase of 19 deaths per day. With a 66 % increase in death year over year, the COVID-19 pandemic in Canada has exacerbated the opioid problem, and we are still learning about the causes and risks that contribute to these terrible overdoses, which involve both prescribed and non-prescribed opioid use.
Why is there an increase in opioid-related harms?
The following reasons may have led to the rise in opioid-related harms:
• Social isolation and pandemic-related stress1
• Erratic unregulated drug supply due to border and travel restrictions1
• Restricted accessibility of healthcare services1
The pandemic has affected virtually all services and therapies accessible to people suffering from chronic pain, addiction, and mental illness.
Anxiety alone is a huge cause for drug use, and what could be more stressful than the current pandemic? People who formerly used drugs with a friend are now doing so alone, with no one to contact 911 or administer naloxone. COVID-19 overburdened emergency rooms and hospitals, and they may not have had the time or resources to address addiction.
Opioids are undeniably effective in the treatment of certain types of pain, such as post-operative, palliative, and cancer pain. However, the fact that around 10% of those who are prescribed opioids go on to develop an opioid use disorder (OUD) is cause for concern2. Furthermore, problematic opioid usage isn't just an individual issue; it's also a 'proximity' issue for friends, family, and communities.
Who are most likely affected by the opioid crisis?
The opioid issue affects some communities and populations disproportionately, such as males aged 20 to 49 who work in the construction industry3. Chronic pain is a major issue in the trades and construction industry, with 32% of workers over-indexing for chronic back pain alone. Construction workers are estimated to account for 30% of all opioid-related deaths. Additionally, workers with a substance use disorder (SUD) miss an average of 14.8 days per year, while workers with OUD miss an average of 29 days per year4. This points to a rise in the number of construction workers seeking treatment for chronic pain and OUD.
Chronic pain, however, is rarely isolated; it is frequently linked with sleep disturbances and emotional distress, forming the well-known "Pain Triad." Opioids are currently the most used drug to treat the Pain Triad. Because no single medication can target all three arms of the pain triad, prescribers frequently turn to multiple high-risk drugs, including opioids, that together increase the abuse potential and worsen symptoms.
As a result, there has been a lot of interest in potential alternatives.
The opioid overdose crisis is worsening during the COVID-19 pandemic with many communities across Canada reporting record numbers of opioid-related deaths, emergency calls and hospitalizations. We can all play a role in supporting those who use substances.
If you or someone you care about is in need of assistance – Get help now.
References:
[1] Special Advisory on the Epidemic of Opioid Overdoses. Opioid and Stimulant-Related Harms in Canada. Ottawa: Public Health Agency of Canada; Sept 2021.
[2] Angus Reid Institute. (2021). Canada’s other epidemic: as overdose deaths escalate, majority favour decriminalization of drugs. Retrieved from https://angusreid.org/wp-content/uploads/2021/03/2021.02.24_Opioid_Dependence.pdf
[3] Gomes, T. et al. Changing Circumstances Surrounding Opioid-Related Deaths in Ontario During the COVID-19 Pandemic. Ontario Drug Policy Research Network / The office of the Chief Coroner of Ontario / Ontario Forensic Pathology Service / Public Health Ontario. May 2021.
[4] Xiuwen, D., Wang, X., Fujimoto, A., & Dobbin, R. (2013). Chronic back pain among older construction workers in the United States: a longitudinal study. International Journal of Occupational and Environmental Health, 18(2), 99-109.